Anxiety and migraine are old friends. When you have migraine, you can’t help worrying: Is my manager going to be upset that I’m missing work again? What does this symptom mean? What happens if I run out of medication this month? Is this attack going to be a really bad one? Will I ever feel normal again? For some people, these migraine-related worries may grow and become an anxiety disorder.

It’s important to note that migraine is a neurological disorder, not (as some think) a psychological condition. However, there seems to be a relationship between migraine and anxiety disorders, scientists have found. Researchers who conducted a review of 178 studies found that epidemiological studies “suggest that patients with migraine – especially those with chronic migraine (CM) and migraine with aura – are at increased risk for major depression, anxiety, or suicidal behavior when compared to subjects without migraine.”
So, does migraine cause anxiety? Or does anxiety cause migraine?
This is a question researchers haven’t been able to answer definitively. Many suggest that the relationship is bidirectional — migraine may increase the likelihood of anxiety, and anxiety, in turn, can exacerbate migraine.

“Notably, the prevalence of anxiety increases with migraine frequency, suggesting a ‘dose-response’ effect; the comorbidity between migraine and anxiety disorders is also enhanced by the presence of medication overuse and concurrent depression,” the researchers above wrote in The Journal of Headache and Pain.
While scientists are trying to illuminate the complex relationship between migraine and anxiety, people living with both conditions are simply trying to manage them. “Anxiety is not just worry and fear, it’s also avoidance that prevents us from doing the things we need and want to do,” migraineur Jennifer writes for Migraine Strong. “It shackles us to our couches pleading for us to avoid everything that creates those worrying thoughts. Sometimes even keeping us from doing the things we love.”
Which anxiety disorders are most often associated with migraine?
There are five main types of anxiety disorders: Generalized Anxiety Disorder (GAD), Obsessive-Compulsive Disorder (OCD), panic disorder, Post-Traumatic Stress Disorder (PTSD), and social phobia.
Many studies have found that people with GAD and panic disorder, in particular, are likely to experience migraines or other types of headaches, according to the Anxiety and Depression Association of America.
People who have Generalized Anxiety Disorder worry a lot about everyday things, have trouble controlling their worries, and know they worry more than they should. Other symptoms include feeling restless, tired and/or irritable; having a hard time concentrating; and having trouble sleeping, among other symptoms.
People who have panic disorder experience sudden, repeated panic attacks. These are characterized by overwhelming anxiety and fear, as well as feelings of being out of control or impending doom. Physical symptoms of a panic attack can include a racing heart, sweating, chills, trembling, breathing problems, weakness or dizziness, tingly or numb hands, chest pain, stomach pain, and nausea.
If you think you may have an anxiety disorder, talk to your healthcare provider about the best ways to treat it. Many people find success with cognitive behavioral therapy (CBT), a form of psychotherapy that teaches new ways of thinking and reacting to situations that cause your anxiety.
Did you know that CEFALY DUAL is now available without a prescription in the U.S. for the preventative and acute treatment of migraine headaches in adults 18 years and older? Try CEFALY DUAL risk-free for 90 days!
How Else Do Migraines Impact Mental Health?
It’s logical to think that migraines could worsen symptoms of anxiety and vice versa. Worry results in stress, and stress is a common migraine trigger. Likewise, the pain and disruption brought on by a migraine can cause feelings of worry, and the cycle continues.
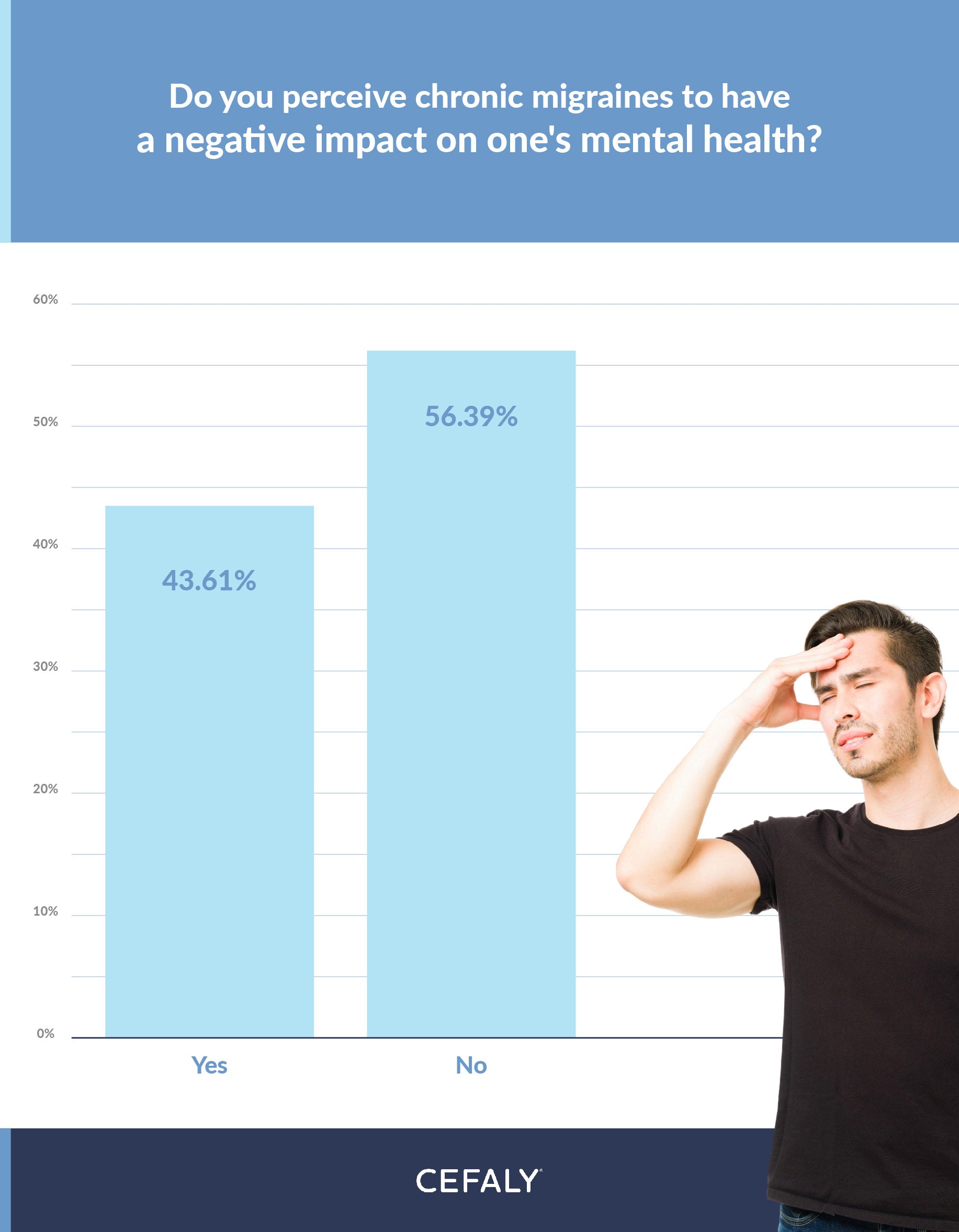
Chronic migraines can also impact mental well-being beyond stimulating feelings of anxiety. Yet it appears many CM sufferers may not be aware of the links between their headaches and mental health. Recent research reveals that over 56% of those surveyed did not perceive an adverse effect of CM on their mental state, while just over 43% did.
The truth is that migraines and mental health are more closely related than one may think. A European study of over 10,000 participants found those who battle migraines reported generally poor mental well-being at more than double the rate of non-migraine sufferers.
According to the American Migraine Foundation, people with episodic or chronic migraines are also five times likelier to have symptoms of depression.
Signs of depression can include:
- Ongoing feelings of sadness, negativity, irritability or helplessness.
- Decreased sense of pleasure in hobbies or interests once found enjoyable.
- Changes in sleeping or eating habits.
- Less energy or increased fatigue.
- Difficulties with focus, memory or making decisions.
- Physical aches and pains that don’t resolve with treatment or have no obvious cause.
Research has also shown that those who have migraines and symptoms of depression are at an increased risk for migraine escalation. In other words, headache sufferers who battle depression may find themselves more likely to progress from episodic migraines to chronic ones, with 15 or more headache days per month.
Further, there is a definitive link between anxiety and depression and higher rates of suicide.
- Increased conversations about death, feeling burdensome or hopeless.
- Excessive use of drugs or alcohol.
- An increase in isolation or social withdrawal.
- Reckless behavior.
If you or a loved one is experiencing these symptoms or contemplating suicide, it’s essential to seek care immediately. Contact your medical professional, a crisis hotline or the National Suicide Prevention Lifeline at 1-800-273-8255 for help.
Other studies have suggested a possible genetic or environmental link between migraines and mental health issues. Research on twins and siblings has discovered that a non-migraine sufferer is more likely to experience depression if their sibling combats migraines. The reverse is also true — the sibling of one who battles with depression has an increased rate of developing migraines.
The medical community remains a bit uncertain as to whether migraine triggers mental health symptoms or vice versa. Yet one thing is clear — it’s vital to recognize and manage the symptoms of both with a proactive treatment plan for better overall physical and mental well-being.
 **The information in this article is not intended to be a substitute for professional medical advice.
**The information in this article is not intended to be a substitute for professional medical advice.
Last Updated May 10, 2022
Dresler, T., Caratozzolo, S., Guldolf, K. et al. Understanding the nature of psychiatric comorbidity in migraine: a systematic review focused on interactions and treatment implications. J Headache Pain 20, 51 (2019). https://doi.org/10.1186/s10194-019-0988-x
